Post Mastectomy Breast Reconstruction in Pottsville, PA
Significant advances have been made in the management of breast cancer over the last 20 years. Improvements in diagnostic techniques and protocols have resulted in progressively earlier detection of breast cancer, which is the most important factor mitigating towards effective treatment and potential cure. Women who carefully follow recommendations for regular breast self exams, periodic breast exams by their gynecologist or family physician and routine screening mammography, benefit from potential diagnosis of early or ‘minimal’ breast cancer and are then eligible for breast conservation treatment. However, for those less fortunate women whose breast cancer is more advanced at the time of initial diagnosis or for whom breast conservation treatment is not appropriate, a modified radical mastectomy may be the optimal treatment. In these situations, post-mastectomy breast reconstruction may represent an excellent therapueutic option.
Although a wide variety of post-mastectomy breast reconstruction techniques exist, they can be broadly divided into two categories: autogenous and prosthetic. Autogenous breast reconstruction involves the use of a patient’s own tissue to reconstruct a breast mound, whereas prosthetic reconstruction involves the use of tissue expanders and implants for breast mound reconstruction. These surgeries can be performed either immediately following mastectomy as part of the same procedure (ie. immediate post-mastectomy breast reconstruction, or at a subsequent time delayed post-mastectomy breast reconstruction’). When performed as an immediate post-mastectomy procedure, patients benefit from the preservation of a greater variety of treatment options and may be eligible for a ‘skin sparing mastectomy’. Following breast mound reconstruction and the completion of any additional necessary breast cancer treatments, such as radiation and/or chemotherapy, patients complete their breast reconstruction in several additional stages including a possible ‘balancing’ procedure on the opposite breast, nipple reconstruction and nipple/areolar tattooing. Due to the many factors affecting the choices in breast reconstruction as well as the variety of reconstructive techniques available, it is not possible to appropriately outline them all in this forum.
Many patients express concern regarding the potential cost of breast reconstructive surgery. However, Federal Legislation adopted in 1998, known as the ‘Women’s Health Care Rights Act’ mandates health insurance coverage for breast reconstruction following mastectomy, including opposite breast ‘balancing’ procedures performed to regain symmetry. This law represents a clear societal commitment to minimize the suffering and disability that can result from mastectomy. Therefore, any woman diagnosed with breast cancer, for whom mastectomy is the recommended treatment, owes it to herself to schedule a consultation with a qualified, experienced plastic surgeon certified by the by the American Board of Plastic Surgery (ABPS). After reviewing prior treatment records, performing a complete history and physical examination and discussing your unique individual concerns, your plastic surgeon can than outline a breast reconstruction plan that is most appropriate for you.
As a board certified plastic surgeon with over 15 years of clinical practice experience and member of the American Society of Plastic Surgeons (ASPS) and American Society of Aesthetic Plastic Surgery (ASAPS-The Mark of Distinction in Cosmetic Plastic Surgery®), Dr. Robert Kimmel welcomes the opportunity to provide breast reconstruction for women who have undergone or who are about to undergo mastectomy. In many situations, breast reconstruction is the key to minimize the physical and psychological trauma that can frequently accompany the loss of a breast. In this way, women are able to more rapidly return to a happy productive lifestyle.
We are proud to serve patients from Scranton, Allentown, and Harrisburg.
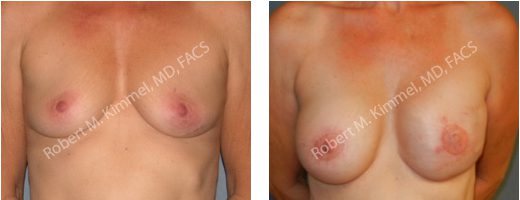
Breast Reconstruction – Before & After
Breast Reconstruction – Before and After Photos
Psychological Benefits of Breast Reconstruction
Breast reconstruction after a mastectomy can offer significant psychological benefits, helping women regain a sense of normalcy and wholeness. The procedure can boost self-esteem and body image, alleviating emotional distress associated with the loss of one or both breasts.
Many women find that breast reconstruction helps them feel more confident in their clothing and social situations, fostering a greater sense of empowerment. Furthermore, it can play a pivotal role in emotional healing, allowing women to close a challenging chapter and move forward with a renewed sense of self.
Immediate vs. Delayed Breast Reconstruction
When considering breast reconstruction, patients have the option of immediate or delayed reconstruction:
Immediate reconstruction is done at the same time as the mastectomy, allowing for the preservation of breast skin and potentially reducing the number of surgeries needed. This option can provide psychological benefits by minimizing the period spent without breasts.
Delayed reconstruction, on the other hand, takes place months or even years after the mastectomy. This may be recommended if the patient requires further cancer treatments, like radiation or chemotherapy, which could affect healing.
The decision between immediate and delayed reconstruction is based on personal preference, overall health, and cancer treatment plans and should be carefully discussed with a plastic surgeon.
Post-operative Care and Recovery for Breast Reconstruction Patients

Frequently Asked Questions
What kind of scarring can I expect after breast reconstruction?
Scarring will depend on the type of reconstruction performed. Most patients will have scars on the breasts and, in some cases, the donor site (if tissue was used from another part of the body). Scars usually fade over time but may not disappear completely.
Will my reconstructed breasts look and feel natural?
Reconstructed breasts can look natural but may feel firmer or less sensitive. The outcome depends on the reconstruction method and individual healing.
How do I prepare for breast reconstruction surgery?
Preparation includes stopping smoking (if applicable), maintaining a healthy diet, and following your surgeon’s guidelines on medications. You may need to adjust any cancer treatments, and your surgeon will provide specific instructions for pre-surgical care.
Can breast reconstruction restore sensation to the breast?
Breast reconstruction typically does not restore full sensation. While some feeling may return over time, most patients experience reduced sensitivity in the reconstructed breast.
What are the different types of breast reconstruction available after a mastectomy?

How does radiation or chemotherapy impact breast reconstruction options?
If you’ve undergone or plan to undergo radiation or chemotherapy, it can influence the timing and type of reconstruction that’s recommended. Radiation can affect skin elasticity and tissue healing, sometimes making flap reconstruction a better choice than implants. In certain cases, reconstruction may be delayed until after your cancer treatments are complete to allow your body to heal fully. Dr. Kimmel collaborates with your oncology team to ensure your reconstruction plan aligns with your overall treatment and recovery process.
Will health insurance cover post-mastectomy breast reconstruction?
In most cases, yes. Federal law requires health insurance plans that cover mastectomies also to cover breast reconstruction, including surgery on the opposite breast for symmetry if needed. This includes all stages of reconstruction, from initial surgery to nipple tattooing or revision work. Keystone Cosmetic Surgery Center will assist you with the insurance process and help ensure that all required documentation is provided.
How long does it take to fully recover from breast reconstruction surgery?
Recovery varies depending on the type of reconstruction performed. Implant-based reconstruction typically takes about 4 to 6 weeks for full recovery, while flap-based procedures may take up to 8 weeks or longer due to additional healing at the donor site. Swelling, tightness, and mild discomfort are common at first, but Dr. Kimmel and his team will guide you through every stage of your recovery with detailed post-operative instructions and follow-up visits.
What’s the difference between immediate and delayed breast reconstruction?
Immediate reconstruction occurs at the same time as the mastectomy, which helps preserve breast skin and avoids an additional surgery later. Delayed reconstruction is performed months or even years afterward, often when additional treatments like radiation are needed. Each option has benefits — immediate reconstruction provides faster aesthetic recovery, while delayed reconstruction allows more flexibility in your overall cancer treatment plan.
How does breast reconstruction support emotional well-being?
For many women, breast reconstruction represents more than physical healing—it’s an important step in emotional recovery. Restoring the shape and symmetry of your breasts can help rebuild confidence, restore femininity, and provide a sense of closure after cancer treatment. Dr. Kimmel takes a compassionate, patient-centered approach to ensure your reconstruction journey supports both your physical and emotional wellness.
What is nipple tattooing, and how does it enhance results?
After reconstruction, nipple tattooing can add realistic color and dimension to the breast for a more natural look. This non-surgical procedure uses medical-grade pigments to create the appearance of the nipple and areola, often as a finishing step in the reconstruction process. Many women find this detail helps them feel whole again after their journey through treatment and recovery.
Feel Like Yourself Again with Breast Reconstruction After Mastectomy in Pottsville, PA
If you are considering breast reconstruction after a mastectomy, our compassionate and experienced team is here to guide you through the process. Take the next step toward restoring your confidence and well-being by scheduling a consultation with our skilled surgeon today. Call our Pottsville office at 570-622-2900 or our Hazleton office at 570-455-4252 to get started.